Types of Crohn’s Disease
Reviewed by: HU Medical Review Board | Last Reviewed: January 2016. | Last updated: October 2019
People with Crohn’s disease have areas of inflammation in the digestive tract. Inflammation leads to symptoms such as diarrhea, abdominal pain, weight loss, or fever.1 Eventually, it can cause serious complications. Complications include narrowing, blockages, areas where pus collects (abscess), or abnormal connections between damaged organs (fistula).1
The type of Crohn's disease depends on what parts of the digestive tract are affected
There are 5 types of Crohn’s disease, based on what parts of the digestive tract are affected (Figure). The location of inflammation is important for many reasons. Your symptoms may be different based on what parts are affected.1 Disease location affects the type of medications or surgery you may need.1
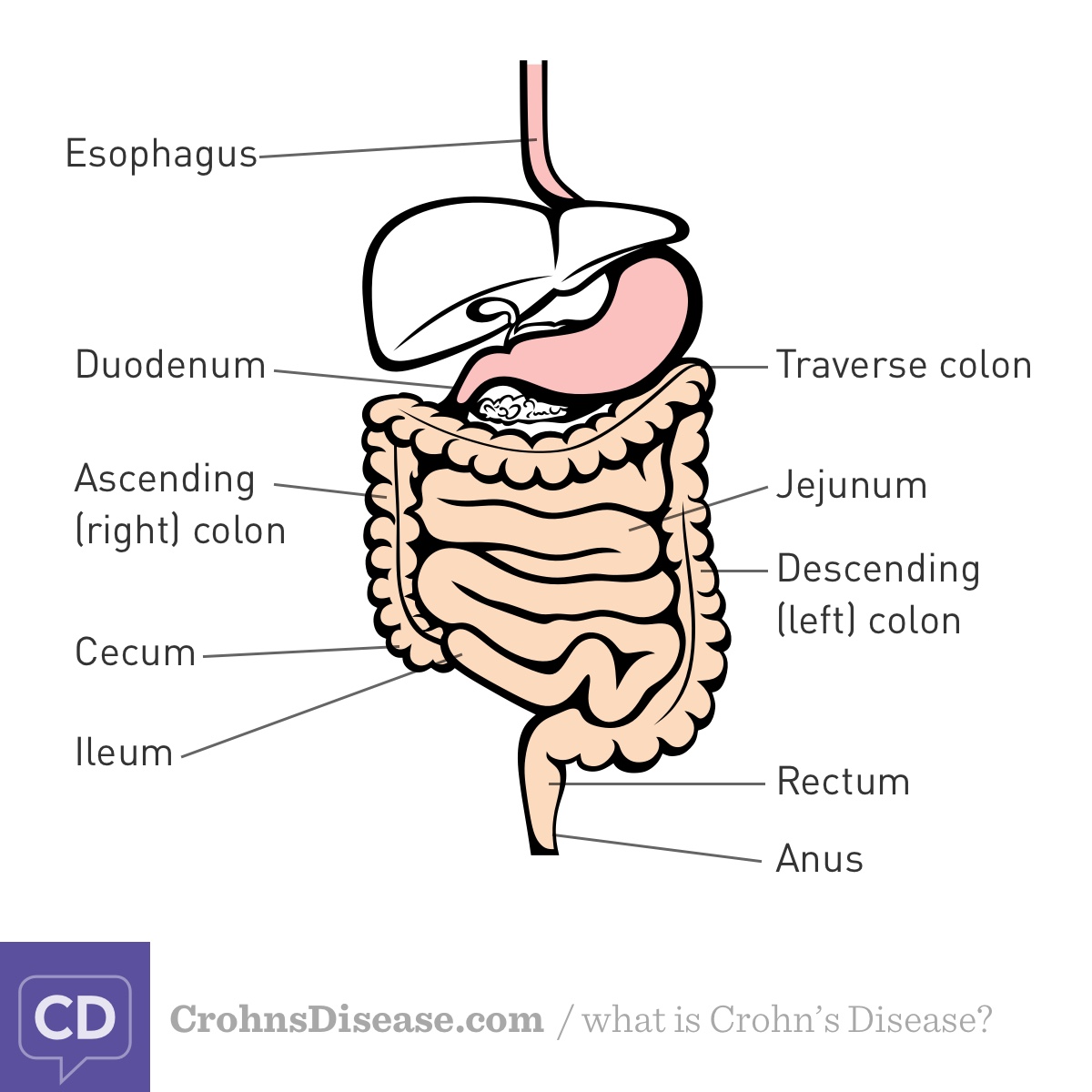
Figure. Terminology
| Term | Where Is That? |
|---|---|
| Esophagus | “Food pipe” that connects your mouth and stomach. |
| Duodenum | First section of the small intestine; starts where the stomach ends. |
| Jejunum | Middle section of the small intestine. |
| Ileum | Last section of the small intestine. |
| Cecum | Pouch at the start of the large intestine, between the ileum and ascending colon. |
| Ascending colon or Right colon | First section of the large intestine. |
| Transverse colon | Second section of the large intestine. |
| Descending colon or Left colon | Third section of the large intestine. |
| Rectum | Last section of the large intestine, connected to the anus. |
| Colorectum | Term that includes all 4 parts of the large intestine. |
Ileocolitis
Ileocolitis is an inflammation of the last part of the small intestine (ileum) and the first part of the colon. You might also hear the term ileoceceal Crohn’s disease. This type of Crohn’s disease is the most common. It affects about 40% of patients.2
You may feel pain in around your belly button or on the lower right side of your abdomen. Most people with ileocolitis have diarrhea.3 It is often watery and unrelated to food intake.4 You may have diarrhea up to 5 times per day.3 Weight loss is common in people with ileocolitis.5 Typical complications are intestinal blockage, inflammatory mass, and abscess.1
Ileitis
Ileitis is inflammation of the ileum, the final part of the small intestine. The symptoms of ileitis are the same as ileocolitis.3 Specifically, people with ileitis usually have pain and diarrhea. Sometimes it is hard to tell ileitis apart from appendicitis, because they cause pain in the same area.1 Symptoms often start 1 to 2 hours after eating a meal.3 Similar to ileocolitis, typical complications are intestinal blockage, inflammatory mass, and abscess.1
Gastroduodenal Crohn's disease
Gastroduodenal Crohn’s disease involves the stomach and first part of the small intestine. The first part of the small intestine is called the duodenum. It is rare to be affected only in the stomach and duodenum.6 Most people with gastroduodenal Crohn’s disease also have inflammation in the ileum and colon.
Typical symptoms of gastroduodenal Crohn’s disease are pain after eating a meal and feeling full quickly. You may lose your appetite or avoid eating because of the pain, which can lead to weight loss.6 It can be hard to tell this type of Crohn’s disease apart from other diseases. Diseases that cause similar symptoms are stomach ulcers, stomach irritation (gastritis), or gastroesophageal reflux disease (GERD).6
Complications of this type of Crohn’s disease can be serious. Bleeding in the stomach or intestine may cause low red blood cell levels (anemia), bloody vomit, or black (tarry) bowel movements.6 If your small intestine becomes blocked, you may feel nauseated or vomit.6
Jejunoileitis
Jejunoileitis is an inflammation of the middle and end of the small intestine. These parts of the small intestine are called the jejunum and ileum. About 20% of children and 4% in adults with Crohn’s disease have this type.7 In one study, 90% of people with jejunoileitis had inflammation in the other parts of the digestive tract as well.8
You may have cramps or diarrhea after eating a meal.7 You may start to lose weight and become malnourished or anemic.7 Children with this type of Crohn’s disease may stop growing. They may go through puberty late.
People with jejunoileitis tend to have more serious complications and need more treatment.7 Blockages in the small intestine can cause nausea or vomiting.7 You may have symptoms outside of the digestive tract, such as arthritis or skin lesions.3
Crohn's (granulomatous) colitis
People with Crohn’s colitis have inflammation in some or all of the colon.9 About 20% of people with Crohn’s colitis are affected only in the colon.10 However, colon inflammation affects about 60% of people with Crohn’s disease.10 A granuloma is a small area of inflamed tissue. About 30% to 45% of people with Crohn’s colitis have granulomas.10,11
Crohn’s colitis causes similar symptoms as ulcerative colitis. It can be hard to tell the 2 conditions apart.3 The main symptom is diarrhea. Inflammation in the colon is more likely to cause bloody diarrhea than inflammation in the small intestine.10
Crohn’s colitis can cause many complications.10 Pus may collect in areas of your colon. This is called an abscess. Abnormal connections can form between the colon and other organs. These connections are called fistulas. Over time, the damage may cause the colon to narrow. People with Crohn’s colitis are more likely to have perianal symptoms.5 Symptoms outside of the digestive tract are common with this type of Crohn’s disease.5
Rare but serious complications include toxic colitis, excessive bleeding (hemorrhage), and tearing (perforations).9,10 People with Crohn’s colitis are at a higher risk of developing colorectal cancer.10