Mucosal Damage
Reviewed by: HU Medical Review Board | Last Reviewed: January 2018.
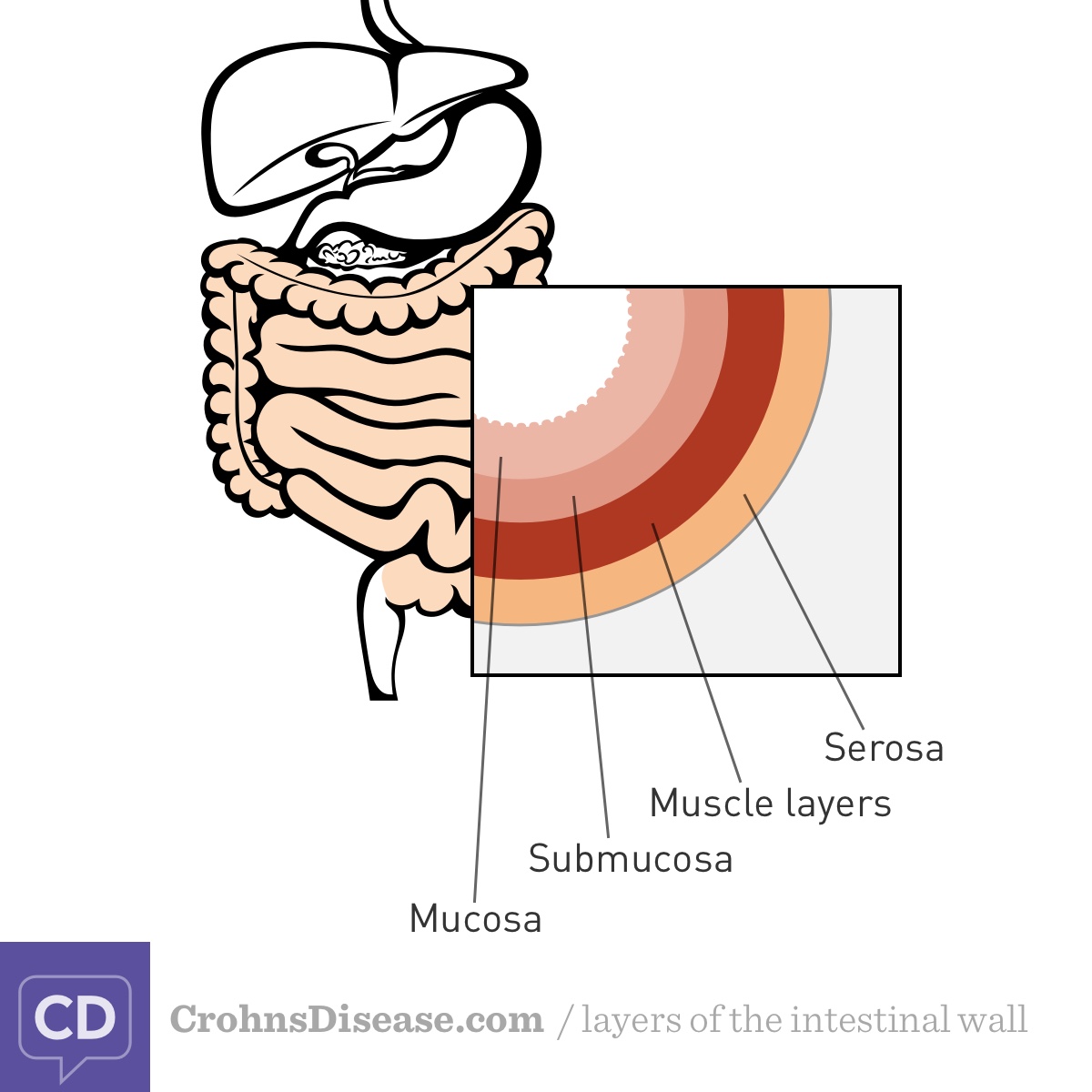
Inflammatory bowel disease (IBD), including Crohn's disease and ulcerative colitis, causes damage to the lining of the digestive tract. The digestive tract is made of several different layers (Figure). Crohn’s disease causes inflammation through all of the layers in patches. Between the damaged areas, the lining may be normal. Ulcerative colitis causes inflammation only in the innermost layer, and the damage is more continuous without the patches seen in Crohn's disease.1 The innermost lining of the digestive tract is called the mucosa or mucous membrane. This layer can be seen using colonoscopy.
Figure. Layers of the intestinal wall
What are signs of mucosal damage?
In mild Crohn’s disease, small canker sores (aphthous ulcers) may be seen in the mucosa.2 The ulcers get progressively worse as disease becomes more severe.2 In moderate Crohn’s disease, the ulcers become larger (stellate ulcers). As inflammation travels deeper into the intestinal wall, the digestive tract begins to look like cobblestones. Large, deep ulcers (serpiginous ulcers) may start to form.
Ulcerative colitis generally begins in the rectum and progresses in a continuous pattern through the colon. Early ulcerative colitis damages the normal blood vessels seen in the mucosa and creates an excess of blood flow to the damaged areas (hyperemia). The inflammation and excess fluid in the area causes the mucosal layer to be very fragile, and it bleeds easily. In moderate ulcerative colitis, ulcers develop. Unlike the ulcers in Crohn's disease, the ulcers seen in ulcerative colitis are surrounded by inflamed mucosa. As the disease progresses, the ulcers can become larger and more continuous.2
Bands of fibrous tissue called strictures are another sign of mucosal damage.3
What other conditions can cause mucosal damage?
Diversion colitis and Behçet's disease are 2 less common inflammatory bowel diseases that can cause ulcers and other damage to the digestive tract.
How is mucosal damage evaluated?
The procedure used to evaluate damage to the digestive tract lining is endoscopy.4 Your doctor performs this procedure using a long, thin tube that has a very small camera with a light at the end. The camera lets your doctor see inside your digestive tract.5 When endoscopy is used to examine the rectum, colon, and ileum, it is called colonoscopy. Endoscopy can also be used to look at upper parts of the digestive tract, including the esophagus, stomach, and beginning of the small intestine.5
How is mucosal damage treated?
Studies have shown that some medications can change the course of IBD. Without treatment, most people progress from inflammation to strictures and fistulas.6
Treatment with biologic medications may change that.4 Biologic medications seem to heal the mucosa. This may prevent complications and improve outcomes.3 A biologic medication may be used with the immunosuppressant azathiprine to help with intestinal healing.4Methotrexate, another immunosuppressant, may be helpful, but it is not the most effective medication for healing the intestine.4 Corticosteroids do not seem to be helpful for this purpose;4 however, they are sometimes used in severe cases to control symptoms while other medications take effect.
What are the benefits of healing the mucosa?
For a long time, the goal of treating IBD was to improve symptoms.7 No one knew whether healing the digestive tract made a difference once the symptoms were under control.4 This changed when biologic medicines were developed. Studies of biologic medications showed that healing the mucosa is beneficial. When the mucosa healed, patients:3,4
- Were more likely to have a period of recovery (remission).
- Needed less medication and surgery.
- Were less likely to be hospitalized.
- Had a better quality of life.
- Were more productive at work.
What are complications of mucosal damage?
A long-term study showed that severe ulcers and damage can lead to more complications and surgery.8 Researchers studied 102 people with Crohn’s disease for more than 4 years. About half of the participants had serious ulcers and lesions at the start of the study. These people were much more likely than others to have fistulas, abscesses, and need surgery.